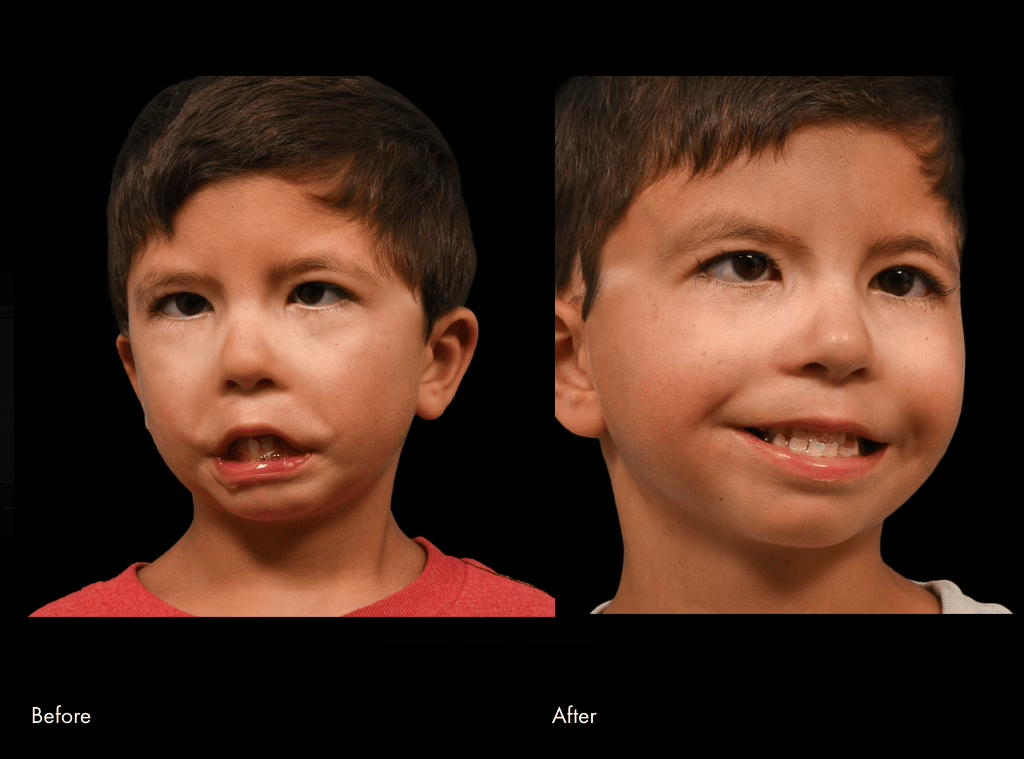
Dealing with facial paralysis in children can be tough. It affects how they smile, talk, and even eat. But there’s hope! Pediatric facial reanimation surgery offers a way to bring back movement and symmetry. This article looks at the whole process, from understanding the problem to seeing the amazing changes after surgery. We’ll cover what you need to know about Pediatric Facial Reanimation Surgery Before & After.
Key Takeaways
- Facial paralysis in kids can impact daily functions and emotional expression, but surgery can help restore movement and symmetry.
- The decision for surgery involves timing, considering both the child’s growth and the need for early intervention for best results.
- Surgical approaches vary, including dynamic methods that transfer muscles for natural movement and static options for support.
- A specialized team approach, advanced imaging, and careful post-operative care are vital for successful outcomes and rehabilitation.
- The results of Pediatric Facial Reanimation Surgery Before & After can significantly improve a child’s quality of life, restoring confidence and social interaction.
Understanding Pediatric Facial Paralysis

Pediatric facial paralysis, commonly referred to as facial palsy, is a condition that affects the proper functioning of the facial muscles, particularly on one side of a child’s face. This impairment can hinder essential facial expressions, such as smiling or frowning, and can complicate basic functions like closing the eyes or controlling saliva. Beyond the physical manifestations, facial paralysis can significantly impact a child’s social interactions and self-esteem, making it a challenging experience for both the child and their family. Various underlying conditions can lead to facial paralysis, ranging from temporary issues like Bell’s palsy to more complex congenital disorders or long-term effects from infections. Understanding the role of the facial nerve, which is responsible for signaling these muscles, is crucial in determining the appropriate treatment options, including potential reanimation surgery. This introduction aims to shed light on the complexities of pediatric facial paralysis, its implications, and the avenues for effective management and support.
How to Talk to My Child About Their Facial Paralysis Condition
The Surgical Journey: Pediatric Facial Reanimation
Embarking on the path of pediatric facial reanimation surgery is a significant step, and understanding the journey ahead is key. This process involves carefully timed interventions designed to restore movement and symmetry to a child’s face.
Timing Considerations for Optimal Outcomes
Deciding when to have surgery is tricky. Usually, a youngster should wait till they’re four, but the timing can vary. For optimal linguistic, social, and facial development, early intervention is recommended. However, waiting too long can be difficult. The idea is to operate when the child’s body is mature enough but early enough to get the best results. Careful consideration ensures the best outcome for your youngster.
Dynamic vs. Static Reanimation Approaches
Dynamic and static facial reanimation methods exist. A muscle with its own blood supply and nerve connection is transferred to the face for dynamic reanimation to restore active movement. This method aims for a spontaneous smile. However, static reanimation supports and balances the face with slings or implants. Static treatments improve immediately but don’t restore active muscle function and may need changes as a child develops. Dynamic methods are more complicated but may yield more natural and durable results.
Microsurgical Muscle Transfer Techniques
One of the most sophisticated methods in dynamic reanimation is the microsurgical muscle transfer. This procedure typically involves taking a small, functional muscle, often from the leg (like the gracilis muscle), and transplanting it to the face. The success hinges on meticulously reconnecting the transferred muscle’s blood vessels and nerves to those in the facial region. This intricate work is performed under a microscope, requiring immense precision. The muscle is then positioned to help create a smile or other facial movements. This complex surgery can take several hours to complete, and post-operative care is intensive, often including a stay in the ICU to monitor the delicate blood vessel connections. This technique is a cornerstone of modern facial reanimation for children.
Pediatric Bell’s Palsy Paralysis Treatments
Preoperative Considerations and Planning

Before any surgical intervention for pediatric facial paralysis, a thorough and careful planning phase is absolutely necessary. This stage involves a multidisciplinary team to assess your child’s specific situation and map out the best path forward. It’s all about getting the details right before we even think about the operating room.
Comprehensive Team Assessment
Your child’s care team will likely include surgeons, neurologists, physical therapists, and possibly speech therapists. They’ll look at how the facial muscles are working (or not working), check for any issues with the eyes or mouth, and consider how the paralysis affects your child’s daily life and communication. This team approach helps ensure all aspects of your child’s health and well-being are considered. We want to make sure we’re not just treating a symptom, but addressing the whole picture.
Advanced Imaging for Precision
Sometimes, we’ll use imaging techniques like MRI or CT scans. These aren’t always needed, but they can give us a clearer view of the facial nerves and surrounding structures. This helps us understand the exact cause and extent of the paralysis, which is really important for planning the most effective surgical strategy. It’s like having a detailed map before starting a journey.
Minimizing Scarring and Disfigurement
Minimizing visible scarring while restoring function is a primary goal in surgical procedures, with surgeons strategically placing incisions to take advantage of natural skin creases and planning for scars that will fade. The approach depends on the child’s age and type of paralysis, opting for conservative management or nerve procedures in young children, while older children may undergo more complex reconstructive techniques, always aiming for optimal outcomes with minimal interventions.
Here’s a general guideline for considering surgical approaches based on age:
- Ages 2-5 years:
- Conservative management is often recommended.
- Nerve repair or transfers are considered if feasible.
- Static procedures (like slings) and regional muscle transfers are generally avoided due to growth.
- Ages 6-21 years:
- Operative intervention becomes more common.
- Static procedures may be performed once growth is mostly complete.
- Nerve procedures remain an option.
- Regional or free muscle transfers are considered based on specific needs and contraindications for microsurgery.
This careful planning is key to achieving the best possible results for your child’s facial reanimation. It’s about setting the stage for success, ensuring that the surgical journey is as smooth and effective as possible, and ultimately helping your child regain facial movement and expression. You can find more information on pediatric surgical procedures that might be relevant.
Postoperative Care and Rehabilitation
Postoperative care and rehabilitation after facial reanimation surgery for children is crucial for successful recovery. Initial monitoring focuses on pain management and following wound care instructions, with activity restrictions, particularly on contact sports, for a few months. Once healing progresses, physiotherapy becomes essential, involving tailored exercises to retrain facial muscles and nerves, with visible movement taking several months to develop. The long-term goals include restoring facial symmetry, emotional expression, and functional abilities like speaking and eating. Follow-up appointments are important for tracking progress and ensuring the best outcomes for the child’s social confidence and interactions.
Here’s a general timeline you might expect:
- Weeks 1-3: Initial healing, wound care, and very gentle movements as advised.
- Month 1-3: Gradual increase in activity, starting physiotherapy exercises.
- Month 4-6: Visible improvements in facial movement begin to appear.
- 6+ Months: Continued progress, with exercises becoming more complex and functional.
The journey of recovery after facial reanimation surgery is a marathon, not a sprint. Patience, consistent effort in physiotherapy, and close collaboration with your medical team are your greatest allies in helping your child achieve their best possible outcome.
Understanding Facial Paralysis Rehabilitation
Potential Complications and Management
Potential complications of pediatric facial reanimation surgery include swelling, minor bleeding, temporary numbness, infection, and rare issues such as flap failure or scar tissue buildup. It is crucial for the surgical team to discuss these risks comprehensively. Revision procedures may be required to address complications or improve results, focusing on enhancing function and aesthetics while considering the child’s growth. The surgery may impact craniofacial growth, but techniques are chosen to be adaptable and minimally invasive, prioritizing the child’s ongoing development and the type of paralysis. Ensuring restoration of function and balance is the primary goal without hindering future growth. We look at:
- The child’s current age and stage of development.
- The specific cause and extent of the facial nerve weakness.
- The potential for the child’s natural recovery over time.
- The long-term goals for facial symmetry and expression.
Managing potential complications and planning for the future are integral parts of the pediatric facial reanimation journey. Open communication with your medical team about expectations and potential challenges is paramount.
While treatments are generally effective, it’s wise to be aware of potential issues. We’ve put together a guide to help you understand what to expect and how to manage any concerns. For more detailed information on managing complications and ensuring the best outcome, visit our website today.
Looking Ahead
Pediatric facial reanimation surgery represents a significant advancement in enhancing the lives of children facing facial challenges. While there are considerations to address throughout the process, the ultimate goal remains clear: to restore not only physical function but also emotional well-being. By enabling better expression, communication, and self-esteem, this surgery can profoundly impact a child’s quality of life. With the support of a dedicated medical team, the journey toward recovery and confidence is not only possible but also transformative, showcasing the remarkable potential of modern medicine.
Request your consultation with Dr. Azizzadeh today
Call us at (310) 657-2203 to schedule an appointment.
Schedule a Consultation